The Key to Health -- A Healthy Lifestyle -- Here Is Our "Formula for Health"

Over the last 10 years there have been 13 major epidemiological studies and one RCT that demonstrate the proposition that just 5 healthy behaviors can avoid the majority of the most common chronic diseases.
The Formula
0 = No cigarettes.
5= 5 servings of fruits and vegetables a day
10=10 minutes of relaxation or stress-reduction each day
30=maintain your BMI under 30, the lower the better
150=150 minutes per week (or roughly 20 minutes a day) of exercise
The Formula
0 = No cigarettes.
5= 5 servings of fruits and vegetables a day
10=10 minutes of relaxation or stress-reduction each day
30=maintain your BMI under 30, the lower the better
150=150 minutes per week (or roughly 20 minutes a day) of exercise
The benefits of such a healthy lifestyle as documented in these studies:
14 Recent Studies from the Medical Literature Show that just these 5 Simple habits can reduce your chance of developing…
Type 2 diabetes by 93%
Hypertension by 78%
Heart Attacks by 83%
Strokes by 79%
Heart failure by 47%
All cancers by 36 to 64%
& reduce your overall chance of dying by 40 to 65%
This is the #1 way to stay healthy and to prevent serious disease!
REFERENCES: (1.) Stampfer
MJ et al. Primary prevention of coronary heart disease in women through diet
and lifestyle. NEJM 2000; 343:6-22; (2.)
Hu FB et al. Diet, lifestyle, and the risk of type 2 diabetes mellitus in
women. NEJM 2001; 345(11):790-7; (3.)
Forman JP et al. Diet and lifestyle risk factors associated with incident
hypertension in women. JAMA 2009; 302(4): 401-11; (4.) Diabetes Prevention Program Research Group. Reduction in the
incidence of type 2 diabetes with lifestyle intervention or metformin. NEJM
2002; 346(6): 393-403; (5.) Knoops
KT et al. Mediterranean diet, lifestyle factors, and 10-year mortality in
elderly European men and women: The HALE project. JAMA 2004; 292: 1433-9; (6.) Yusuf S et al. Effect of
potentially modifiable risk factors associated with myocardial infarction in 52
countries (the INTERHEART study): case-control study. Lancet 2004; 364: 937-52;
(7.) Kurth T et al. Healthy
lifestyle and the risk of stroke in women. Archives of Internal Medicine 2006;
166: 1403-9; (8.) Chiuve SE et al.
Healthy lifestyle factors in the primary prevention of coronary heart disease
among men: benefits among users and nonusers of lipid-lowering and
antihypertensive medications. Circulation 2006; 114: 160-7; (9.) Chiuve SE et al. Primary
prevention of stroke by healthy lifestyle. Circulation 2008; 118: 947-54; (10.) Djousse L et al. Relation between
modifiable lifestyle factors and lifetime risk of heart failure. JAMA 2009;
302(4): 394-400; (11.) King DE et
al. Turning back the clock: adopting a healthy lifestyle in middle age.
American Journal of Medicine 2007; 120: 598-603; (12.) Khaw KT et al. Combined impact of health behaviours and
mortality in men and women: the EPIC-Norfolk prospective population study. PLoS
Med 2008; 5(1):e12; (13.) Ford ES et
al. Healthy living is the best revenge: Findings from the European Prospective
Investigation into Cancer and Nutrition—Potsdam Study. Arch Intern Med 2009;
169(15):1355-62; (14.) Lee C et al.
Combined effects of cardiorespiratory fitness, not smoking, and normal
waist:girth on morbidity and mortality in men. Arch Intern Med 2009; 169(22):
2096-2101.
Latest issue...
FP Revolution
Dawn of a New Age of Health Information
published by www.Kopes-eticHealth.com
http://DrLifestylesEvidenceforHealth.blogspot.com
Colin P Kopes-Kerr, MD
Eastern Plumas Health Care Portola CA
[email protected]
FP Revolution Volume 5 Number 2 February 28, 2011
KEY WORDS
SUN SCREEN SKIN CANCER
TANNING USPSTF
GUIDELINES DIET
EXERCISE HEPATITIS C
CIRRHOSIS HCC
COMORBIDITY PSA
PROSTATE CANCER ULTRASOUND
CONFLICT OF INTEREST CT SCANS
KIDNEY STONES RADIATION
EXERCISES IN LOGIC
SHOULD WE COUNSEL PATIENTS TO USE SUN SCREEN, AVOID TANNING? Here is what the USPSTF concludes in a recent guideline update: ""Randomized, controlled trials suggest that primary care-relevant counseling can increase sun-protective behaviors and decrease indoor tanning." What does this say to you? It leaves me waiting to hear the point--"and so we should do what?" There is a reason this conclusion is so vague. They don't have much data to go on (despite their alleged RCTs). Here are some of the basic facts they had to work with:(1)
- In 2003 the USPSTF had concluded that "evidence was insufficient" to recommend for or against routine counseling by primary care physicians to prevent skin cancer because of the uncertainty surrounding whether clinician counseling is effective in changing patient behaviors to reduce skin cancer, the uncertainty about potential harms of sun-protective behaviors, and availability of only fair-quality evidence linking sunscreen use or indoor tanning to skin cancer outcomes."
- "We found no trials meeting our inclusion criteria that directly examined whether behavioral counseling interventions can reduce skin cancer."
- Among 335 unique fair- or good-quality studies evaluating the epidemiological association between sun exposure, indoor tanning, or sunscreen use and skin cancer, they were only able to find 1 good-quality trial, the Nambour Skin Cancer and Actinic Eye Disease Prevention Trial.
- "Although few studies examined the association between total (or cumulative) and chronic (or occupational) sun exposure, most existing studies did not suggest a strong association between total or chronic sun exposure and squamous cell carcinoma or basal cell carcinoma...On the basis of fair quality case-control studies, it seems that both total and chronic sun exposure are not as strongly associated with melanoma...These studies showed mixed results: Two studies found a statistically significant association between total lifetime sun exposure and melanoma and 4 did not."
- "Five fair-quality case-control studies examined the association between indoor tanning and the risk for squamous cell carcinoma or basal cell carcinoma...and none of these studies found a statistically significant association between ever and never use."
- "We found one RCT examining whether regular sunscreen use can prevent squamous cell carcinoma or basal cell carcinoma. After 8 years of follow-up, persons randomly assigned to regular sunscreen use had a decreased risk (risk ratio, 0.65) for squamous cell carcinoma, but not basal cell carcinoma. Two fair quality cohort studies from he Nurses' Health Study did not show a decrease in squamous cell carcinoma or basal cell carcinoma risk with sunscreen use...On the basis of one fair-quality cohort and 4 fair-quality case-control studies, sunscreen use has no clear protective or harmful effect on the risk for melanoma...Two studies conducted in Sweden found a statistically significant harmful effect of sunscreen, such that persons who reported always or almost always using sunscreen were at increased risk for melanoma, after adjustment for both skin phenotype and sun exposure."
- On the benefits of intervention they say, "Evidence in adults and parents of newborns suggests that behavioral interventions can minimally increase composite scores measuring sun protective behaviors. [Whoopee!] It is unclear, however, whether the small differences in composite scores of self-reported sun-protective behaviors translate into clinically meaningful behavior change to prevent skin cancer or sunburns." [Isn't this exactly what we were after?]
- "More and better studies are needed."
A MEDITATION ON DIET AND EXERCISE: "Our Paleolithic ancestors lived in small bands of roaming hunter-gatherers. Living like this, our ancestors must have had a very, very active life: roaming, hunting, gathering, and avoiding being eaten by various carnivores. Their DNA would have been modeled by millennia of natural selection to adapt them to this very active lifestyle. Thus, because our own current genetic heritage contains DNA like that of our Paleolithic forbearers, we, too, have a genetic makeup that demands (or is well suited to?) an active lifestyle. "The conclusion from this thought experiment is evident: our DNA heritage with its highly complex biochemical and physiological processes is appropriate to a very active lifestyle, not a modern 21st century couch potato, fast-food existence. Consequently, we should make every effort to include elements that resemble the Paleolithic lifestyle in our modern daily existence. My lifestyle included daily exercise, lots of fruits and vegetables in the diet, and avoidance of heavily engineered snack food. Or course, I also do not smoke tobacco nor do I consume large quantities of alcohol. I recommend these lifestyle elements to all my patients. When friends of family ask, 'How often should I exercise?' my answer is always 'Only on the days you eat.' That seems to get the message across."(2) COMMENT: Well said.
MORE ILLOGIC FROM THE VETERANS ADMINISTRATION ON THE TOPIC OF HEPATITIS C AND SURVEILLANCE FOR HEPATOCELLULAR CARCINOMA: Let's do our standard analysis and start with the conclusion: "Few HCV-infected veterans with cirrhosis received routine HCC surveillance. New strategies are needed to improve the implementation of HCC surveillance." Does this seem reasonable to you? While I do suspect that few such patients receive this surveillance, I doubt that new strategies are needed to improve such surveillance. The problem is that no randomized, controlled trials of HCC surveillance have been done in HCV-infected patients. The rationale for the published guidelines calling for HCC surveillance with AFP and ultrasound is that it has been demonstrated to be somewhat effective for chronic hepatitis B infection in Japan, which is a different disease. When the Cochrane group reviewed this issue in 2009 (4), they concluded from a review of 18,816 patients who were randomized to biannual AFP plus US versus no screening for 5 years that this evidence was insufficient to justify any recommendation at this time. [See FP Revolution, 2010 4: No 4: Melissa Wong.] The number of patients diagnosed with HCC was increased in the screened group (OR 1.37, 95% CI 1.00-1.88), but there was no difference in HCC mortality (OR 0.81, 95% CI 0.54-1.22). All-cause mortality was not reported. COMMENT: Why our obsession with increasing clinical (expensive) behaviors that are not proven effective?
MORE TRASH LITERATURE FOR THE BENEFIT OF THE PSA PEOPLE: A very curious article appeared last year in the oncology literature. The data came from the well-respected Prostate, Lung, Colorectal and Ovarian PC screening study.(4) The only problem is that this report is merely a post-randomization subgroup analysis. What they found was that, after 10 years of follow-up, there was a significant decrease in the risk of prostate cancer-specific mortality (22 vs 38 deaths; adjusted hazard ratio, 0.56; P=an exciting 0.03) in men with no or minimal comorbidity randomly assigned to intervention vs usual care; this led to a calculated NNT to prevent one prostate cancer death at 10 years of 5. Among men with at least one significant comorbidity, those randomly assigned to intervention vs usual care did not have any decrease in risk of prostate-cancer-specific mortality. It is a very interesting idea to stratify the results of cancer screening program by differing levels of associated comorbidities (e.g., in the feeble, debilitated elderly there is no point to colon cancer screening, prostate cancer screening, breast cancer screening, or cervical cancer screening). In this study they developed an unusual definition of "comorbidity"--"a comorbidity was defined as one that could increase the risk of dying from one of the two leading causes of death in the US for men between the ages of 55 and 74 years (i.e., cardiovascular disease or cancer)." For cardiovascular disease, the specific comorbidities included known coronary heart disease and/or myocardial infarction [no one will argue about the appropriateness of these criteria] and "risk factors such as hypertension, diabetes, stroke, and obesity (BMI > 30 kg/m2). For cancer, specific medical conditions that increase the risk of developing a non-prostate cancer were included--ulcerative colitis, Crohn's disease, familial polyposis syndrome/Gardner's syndrome, diverticulitis, diverticulosis, gallbladder stones/inflammation, colorectal polyps, bronchitis, emphysema, cirrhosis of the liver, and hepatitis." [These criteria, alas, are ones that no reasonable doctor would use as a meaningful variable to select patients for cancer prevention interventions. They are simply nuts.] The problem, of course, is that once you define "comorbidity" this broadly you have included just about everyone in the population. In fact, only 35.7% of their population could be classified as either "no comorbidity" or "minimal comorbidity". [Query: It is not even clear, using their definition, what "minimal comorbidity" means.] Furthermore, among the subjects studied by the end of the sixth year there was a 52% contamination rate in the group assigned to usual care (i.e., they received PSA screening anyway).
The one part of this report that a critical reader cannot fault is this part of their conclusion: "The association between a significant reduction in the risk of prostate cancer-specific mortality in men with no or minimal comorbidity as defined in this study and randomly assigned to intervention compared with the usual care arm is hypothesis generating, given that this was a post-randomization analysis." Furthermore, "People who participate in screening studies are generally more healthy and more health conscious than nonattendees, meaning that the 35.7% estimate of men with no or minimal comorbidity in this study may be an overestimate when applied to the general population." COMMENT: This is a pure junk study in a shrinking market for PSA. It is clear that it is not yet clinically cost-effective; for the morbid elderly it is extraordinarily clear that it is not indicated. The authors seem to be trying to hold on to a small niche of apparently healthy people, but massive amounts of other data demonstrate, even for this group, that there is no value to PSA screening. Simply put, we need a different test, if we are to screen for prostate cancer.
DOES INDUSTRY AFFECT OUR MEDICAL LITERATURE? Of course it does. Disclosure of conflict-of-interest for publication is just one small aspect of the problem, but it is a concern. How much confidence can you place in the required disclosures of relationships with industry now required for publication? While the journals require disclosure, they currently do nothing to verify their accuracy. Congress is considering legislation that would require public records of all payments made to physicians. This study from Harvard analyzed the accuracy of disclosure by physicians who were presenters or who served as board or committee members for the 2008 annual meeting of the American Academy of Orthopedic Surgeons and who had received payments (monetary or in-kind) in 2007 from 5 manufacturers of hip or knee prostheses.(6) The five companies had made 1,347 payments to 1,162 physicians in 2007, and one-fourth of these payments (344) were made to presenters or board/committee members of the annual orthopedic meeting (69.6% of these payments were judged to be directly related to the topic of the meeting presentations). Rates of disclosures printed in the final meeting program were 71.2% overall and 79.3% for payments that were directly related to the meeting presentation. Surveys were distributed to 91 physicians who did not disclose industry payments in the annual meeting program. Among the 36 responding physicians (39.6%) reasons cited for nondisclosure included the belief that payments were unrelated to the topic of their presentations and misunderstanding of disclosure requirements. COMMENT: We have gotten so good at lying to ourselves that we are able to forget why companies give us this money in the first place. They want something.
PRACTICAL QUESTION: WHICH IS BETTER FOR THE CONFIRMATION OF A KIDNEY STONE -- CT OR ULTRASOUND? Ultrasound has a lower sensitivity than CT scanning for diagnosing urolithiasis in adults, but is less expensive and does not carry the substantial risk of ionizing radiation associated with CT scanning; this is particularly important in a disease expected to be recurrent and thus requiring repeated imaging. This study is a prospective study among children from Children's Hospital in Boston. The authors analyzed the results from 50 children less than 18 years of age with signs, symptoms or a history suggestive of urolithiasis; all children had both studies. Nephrolithiasis was diagnosed on CT in 34 patients (68%), and it was also found on ultrasound in 26 of these 34, and in one of the others (sensitivity and specificity of US, 76% and 100%). Of the 8 patients with a false-negative US, only 4 received specific therapy for the stone and all 4 had US findings of hydronephrosis. These authors suggest that these ultrasound results are "good enough" given the costs and radiation exposure associated with CT scanning. They suggest that ultrasound be the primary imaging modality for suspected kidney stones. COMMENT: This makes a great deal of sense. The medical profession has been slow overall to react appropriately to the radiation risk inherent in using CT scans. This is especially true for a condition where repeated imaging is likely to be necessary, and most particularly so for children. Where I last worked, the urologists wouldn't see a patient with recurrent kidney stone unless a CT scan had been performed. Remember that we don't really care about small stones. The important stones to recognize are the ones causing obstruction and ultrasound should be just fine for this indication.
REFERENCES:
1. Lin JS et al. Behavioral counseling to prevent skin cancer: A systematic review for the US Preventive Services Task Force. Ann Intern Med 2011; 154: 190-201. ÂÂ
2. Alpert JS. You only have to exercise on the days that you eat. Am J Med 2011; 124: Editorial. doi:10.1016/j.amjmed.2010.09.004 ÂÂ
3. Wun YT, Dickinson JA. Alpha-fetoprotein and/or liver ultrasonography for liver cancer screening in patients with chronic hepatitis B. Cochrane Database of Systematic Reviews 2003, Issue 2. Art. No.: CD002799. ÂÂ
4. Davila JA et al. Utilization of surveillance for hepatocellular carcinoma among hepatitis C virus-infected veterans in the United States. Ann Intern Med 2011; 154: 85-93. ÂÂ
5. Crawford ED et al. Comorbidity and mortality results from a randomized prostate cancer screening trial. J Clin Oncol 2010; 28: DI: 10.1200/JCO.2010.30.5979 ÂÂ
6. Okike K et al. Accuracy of conflict-of-interest disclosures reported by physicians. E Engl J Med 2009; 361:1466. ÂÂ
7. Passerotti C et al. Ultrasound versus computerized tomography for evaluating urolithiasis. J Urol 2009; 182 (4 Suppl): 1829; abstracted in Emerg Med Abstracts 2010; 3/10: #24. ÂÂ
BACK ISSUES of FP Revolution may be found at: http://kopes-etichealth.icontact.com/archives/kopes-etichealth TO ORDER FP REVOLUTION just send an e-mail to [email protected] with "SIGN UP" in the subject line. FP Revolution is a free weekly clinical e-zine sent to those who request it. If you feel that you have received this in error, please click on the link below to have your name removed from this list. Dr. Kopes-Kerr currently practices with the Eastern Plumas Health Care, Portola, CA. The opinions expressed in this newsletter represent solely the views of Dr. Kopes-Kerr and are not intended in any way to represent the opinions or policies of the Eastern Plumas Health Care.
Latest issue...March 31, 2011
FP Revolution
Dawn of a New Age of Health Information
published by www.Kopes-eticHealth.com
http://DrLifestylesEvidenceforHealth.blogspot.com
Colin P Kopes-Kerr, MD
Eastern Plumas Health Care Portola CA
[email protected]
FP Revolution Volume 5 Number 3 March 31, 2011
KEY WORDS
PYELONEPHRITIS UTI
SHORT COURSE THERAPY AUGMENTIN
OTITIS MEDIA DVT
PULMONARY EMBOLISM PROPHYLAXIS
published by www.Kopes-eticHealth.com
http://DrLifestylesEvidenceforHealth.blogspot.com
Colin P Kopes-Kerr, MD
Eastern Plumas Health Care Portola CA
[email protected]
FP Revolution Volume 5 Number 3 March 31, 2011
KEY WORDS
PYELONEPHRITIS UTI
SHORT COURSE THERAPY AUGMENTIN
OTITIS MEDIA DVT
PULMONARY EMBOLISM PROPHYLAXIS
PRACTICAL MEDICINE
HOW LONG IS ENOUGH FOR TREATMENT OF UTI IN THE ELDERLY? This is a common enough occurrence that we might as well do it right. Studies have adequately compared single-dose therapy, to short course-therapy (3-6 days), and to long-course therapy (7-14 days). Both short-course and long-course treatment are superior to single-dose therapy (twice as many patients cured). Long-course treatment, however, offers no additional benefit compared to short-course therapy.(1) COMMENT: And there you have it--a simple clear answer. There's no reason to be using 7-14 days of antibiotics for these folks. My preference is for 5 days.
HOW LONG IS ENOUGH FOR TREATMENT OF ACUTE PYELONEPHRITIS? A recent meta-analysis of 4 RCTs on acute pyelonephritis involving 199 patients--mostly adult women ages 16 to 94 years. The authors found no significant differences in clinical success rates between short (7-14 days) and long (14-42 days) course of antibiotic treatment for acute pyelonephritis. A recent evidence-based guideline from ACOG on the treatment of pyelonephritis in non-pregnant women recommends 14 days of total antibiotic treatment (either inpatient or outpatient).(2) COMMENT: I had no idea that anyone had ever treated pyelonephritis for 6 weeks. How bizarre!
EAR INFECTIONS IN CHILDREN: TO TREAT OR NOT TO TREAT? A brief history of ear infections (otitis media) is in order before going on to intelligently review the current state of the art. Once upon a time that a few of us still alive (but not myself) well remember, there were no antibiotics, and recurrent ear infections in children were a serious problem. Untreated, they could lead to mastoiditis, meningitis, and even death. When antibiotics came along, the attitude was "Of course, we'll treat. This is a bad disease." And treatment worked. Mastoiditis became a rare problem. Meningitis became even more rare, especially after new vaccines. Ultimately, ear infections in children became a very benign and simple problem. For the last 50 years or so, there have been hundreds of studies comparing every new antibiotic made by a pharmaceutical company to the old traditional ones trying to show that the new one was better in some way--either it cured more cases or had fewer side effects. The general lesson we have learned from these studies is that the choice of antibiotic doesn't make much difference, so you just use the least expensive one.
Then, a funny thing happened in the 1970s. Since otitis media was becoming a minor illness with just a few days of fussiness and moderate discomfort which would in the majority of cases go away even if it was not treated, European investigators started asking the question or whether you really need antibiotics at all for this newly less serious infection. The Netherlands pioneered this effort, and there it became standard policy NOT to treat ear infections with antibiotics at the first visit. At the first visit doctors would just recommend Tylenol and analgesic drops (like Auralgan) in the ears. Then parents were given instructions that if symptoms were not much better by 3 days, they should return to get antibiotics. It turns out that this policy worked very well. The overall cure rates were the same as in the US, where antibiotics were being used routinely, and there were no increases in complications like mastoiditis.
It took a while for this approach to drift over to the US, but in the 80s and early 90s there were a number of studies that compared antibiotic treatment of otitis media to the outcomes in children who were not treated with antibiotics. What these studies showed consistently is that there was a small, statistically significant, short-term benefit in the children who were treated with antibiotics. The precise benefit was one day less of symptoms (shorter duration of illness) in 1 out of 7 children treated. This was shocking, of course, to physicians who were trained to treat ear infections. Thus, despite the very clear literature, only a minority of physicians actually stopped prescribing antibiotics; old habits die hard. In my practice I have always preferred to share the evidence with the patients (in this case, t he parents) and let them make their own decision. I neither urged nor discouraged antibiotic use. Instead I asked the parents if they would want to use antibiotics for their child for the sake of possibly (a 1 in 7 chance) having one day less of symptoms at the risk of a drug reaction, most commonly a rash, upset stomach, or diarrhea. In my experience about 75% of parents chose to use the antibiotic. Since the 1990s there have been very few studies of ear infections in children and absolutely no change in the bottom line--antibiotics confer a 1 in 7 chance of 1 day less of symptoms. This is why it is a noteworthy event that 2 recent studies have just been published in the New England Journal of Medicine on the treatment of ear infections in children--one in children less than 2 years of age in Pittsburgh PA, (3) and the other in children aged 6 to 35 months in Finland. (4) They both reach the same conclusion--that the benefits of antibiotic treatment are greater than has previously been estimated.
Let's take a look at those two studies and see how convincing this conclusion is.
In the under-2 years of age study, 291 children aged 6 to 23 months were diagnosed by experts using stringent criteria for the diagnosis of ear infection, and when an ear infection was diagnosed one group received a potent antibiotic (Augmentin) and the other group received a placebo. Among the children who received Augmentin (amoxicillin-clavulanate), 35% had initial resolution of symptoms by day 2, 61% by day 4, and 80% by day 7. This compared to rates of 28% resolution by day 2, 54% resolution by day 4, and 74% resolution by day 7. These small differences were NOT statistically significant. For sustained relief of symptoms, the rates were 20% vs 14% at 2 days, 41% vs 36% at 4 days, and 67% vs 53% at 6 days. This result achieved borderline statistical significance (P value=0.04). Mean symptoms scores over the first 7 days were lower for the children treated with antibiotics than for those who received placebo (P=0.02). The rate of clinical failure, defined as the persistence of signs of acute infection on otoscopic examination, was also lower among the children treated with antibiotics than among those who received placebo: 4% vs 23% at or before the visit on day 4 or 5 (P < 0.001) and 16% vs 51% at or before the visit on day 10 to 12 (P < 0.001).
The second study randomized 319 children aged 6 to 35 months in Finland who were diagnosed by strict criteria as having ear infections to either placebo or the same antibiotic as above. Treatment "failure" occurred in 18.5% of the children who received the antibiotic vs 44.9% of the children were received placebo (P < 0.001). At 3 days after diagnosis, the failure rate was 13.7% in the antibiotic group vs. 25.3% in the placebo group. Overall, the antibiotic reduced the progression to treatment failure by 62%. Side-effects were much more common in the antibiotic group, and 47.8% of the treated children experienced diarrhea. The authors of this study comment, "Future studies should identify patients who may derive the greatest benefit, in order to minimize unnecessary antimicrobial treatment and the development of bacterial resistance." An editorialist reviewing these two studies concludes: "Is acute otitis media a treatable disease? The investigators in Pittsburgh and Turku, Finland have provided the best data yet to answer the question, and the answer is yes; more young children with a certain diagnosis of acute otitis media recover more quickly when they are treated with an appropriate antimicrobial agent." (5)
HOW LONG IS ENOUGH FOR TREATMENT OF UTI IN THE ELDERLY? This is a common enough occurrence that we might as well do it right. Studies have adequately compared single-dose therapy, to short course-therapy (3-6 days), and to long-course therapy (7-14 days). Both short-course and long-course treatment are superior to single-dose therapy (twice as many patients cured). Long-course treatment, however, offers no additional benefit compared to short-course therapy.(1) COMMENT: And there you have it--a simple clear answer. There's no reason to be using 7-14 days of antibiotics for these folks. My preference is for 5 days.
HOW LONG IS ENOUGH FOR TREATMENT OF ACUTE PYELONEPHRITIS? A recent meta-analysis of 4 RCTs on acute pyelonephritis involving 199 patients--mostly adult women ages 16 to 94 years. The authors found no significant differences in clinical success rates between short (7-14 days) and long (14-42 days) course of antibiotic treatment for acute pyelonephritis. A recent evidence-based guideline from ACOG on the treatment of pyelonephritis in non-pregnant women recommends 14 days of total antibiotic treatment (either inpatient or outpatient).(2) COMMENT: I had no idea that anyone had ever treated pyelonephritis for 6 weeks. How bizarre!
EAR INFECTIONS IN CHILDREN: TO TREAT OR NOT TO TREAT? A brief history of ear infections (otitis media) is in order before going on to intelligently review the current state of the art. Once upon a time that a few of us still alive (but not myself) well remember, there were no antibiotics, and recurrent ear infections in children were a serious problem. Untreated, they could lead to mastoiditis, meningitis, and even death. When antibiotics came along, the attitude was "Of course, we'll treat. This is a bad disease." And treatment worked. Mastoiditis became a rare problem. Meningitis became even more rare, especially after new vaccines. Ultimately, ear infections in children became a very benign and simple problem. For the last 50 years or so, there have been hundreds of studies comparing every new antibiotic made by a pharmaceutical company to the old traditional ones trying to show that the new one was better in some way--either it cured more cases or had fewer side effects. The general lesson we have learned from these studies is that the choice of antibiotic doesn't make much difference, so you just use the least expensive one.
Then, a funny thing happened in the 1970s. Since otitis media was becoming a minor illness with just a few days of fussiness and moderate discomfort which would in the majority of cases go away even if it was not treated, European investigators started asking the question or whether you really need antibiotics at all for this newly less serious infection. The Netherlands pioneered this effort, and there it became standard policy NOT to treat ear infections with antibiotics at the first visit. At the first visit doctors would just recommend Tylenol and analgesic drops (like Auralgan) in the ears. Then parents were given instructions that if symptoms were not much better by 3 days, they should return to get antibiotics. It turns out that this policy worked very well. The overall cure rates were the same as in the US, where antibiotics were being used routinely, and there were no increases in complications like mastoiditis.
It took a while for this approach to drift over to the US, but in the 80s and early 90s there were a number of studies that compared antibiotic treatment of otitis media to the outcomes in children who were not treated with antibiotics. What these studies showed consistently is that there was a small, statistically significant, short-term benefit in the children who were treated with antibiotics. The precise benefit was one day less of symptoms (shorter duration of illness) in 1 out of 7 children treated. This was shocking, of course, to physicians who were trained to treat ear infections. Thus, despite the very clear literature, only a minority of physicians actually stopped prescribing antibiotics; old habits die hard. In my practice I have always preferred to share the evidence with the patients (in this case, t he parents) and let them make their own decision. I neither urged nor discouraged antibiotic use. Instead I asked the parents if they would want to use antibiotics for their child for the sake of possibly (a 1 in 7 chance) having one day less of symptoms at the risk of a drug reaction, most commonly a rash, upset stomach, or diarrhea. In my experience about 75% of parents chose to use the antibiotic. Since the 1990s there have been very few studies of ear infections in children and absolutely no change in the bottom line--antibiotics confer a 1 in 7 chance of 1 day less of symptoms. This is why it is a noteworthy event that 2 recent studies have just been published in the New England Journal of Medicine on the treatment of ear infections in children--one in children less than 2 years of age in Pittsburgh PA, (3) and the other in children aged 6 to 35 months in Finland. (4) They both reach the same conclusion--that the benefits of antibiotic treatment are greater than has previously been estimated.
Let's take a look at those two studies and see how convincing this conclusion is.
In the under-2 years of age study, 291 children aged 6 to 23 months were diagnosed by experts using stringent criteria for the diagnosis of ear infection, and when an ear infection was diagnosed one group received a potent antibiotic (Augmentin) and the other group received a placebo. Among the children who received Augmentin (amoxicillin-clavulanate), 35% had initial resolution of symptoms by day 2, 61% by day 4, and 80% by day 7. This compared to rates of 28% resolution by day 2, 54% resolution by day 4, and 74% resolution by day 7. These small differences were NOT statistically significant. For sustained relief of symptoms, the rates were 20% vs 14% at 2 days, 41% vs 36% at 4 days, and 67% vs 53% at 6 days. This result achieved borderline statistical significance (P value=0.04). Mean symptoms scores over the first 7 days were lower for the children treated with antibiotics than for those who received placebo (P=0.02). The rate of clinical failure, defined as the persistence of signs of acute infection on otoscopic examination, was also lower among the children treated with antibiotics than among those who received placebo: 4% vs 23% at or before the visit on day 4 or 5 (P < 0.001) and 16% vs 51% at or before the visit on day 10 to 12 (P < 0.001).
The second study randomized 319 children aged 6 to 35 months in Finland who were diagnosed by strict criteria as having ear infections to either placebo or the same antibiotic as above. Treatment "failure" occurred in 18.5% of the children who received the antibiotic vs 44.9% of the children were received placebo (P < 0.001). At 3 days after diagnosis, the failure rate was 13.7% in the antibiotic group vs. 25.3% in the placebo group. Overall, the antibiotic reduced the progression to treatment failure by 62%. Side-effects were much more common in the antibiotic group, and 47.8% of the treated children experienced diarrhea. The authors of this study comment, "Future studies should identify patients who may derive the greatest benefit, in order to minimize unnecessary antimicrobial treatment and the development of bacterial resistance." An editorialist reviewing these two studies concludes: "Is acute otitis media a treatable disease? The investigators in Pittsburgh and Turku, Finland have provided the best data yet to answer the question, and the answer is yes; more young children with a certain diagnosis of acute otitis media recover more quickly when they are treated with an appropriate antimicrobial agent." (5)
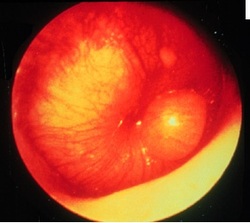
Fig 1: An acute ear infection: a very bulging tympanic membrane.
COMMENT: To all this I have to say, "Not so fast!" First, the authors used, as is appropriate for a formal study, a "strict" definition of an ear infection. In the Finnish study, three overall criteria were required for the diagnosis of acute otitis media (see videos 1, 2, and 3). First, middle-ear fluid had to be detected by means of pneumatic otoscopic examination that showed at least two of the following tympanic-membrane findings: bulging position, decreased or absent mobility, abnormal color or opacity not due to scarring, or air–fluid interfaces. Second, at least one of the following acute inflammatory signs in the tympanic membrane had to be present: distinct erythematous patches or streaks or increased vascularity over full, bulging, or yellow tympanic membrane. Third, the child had to have acute symptoms, such as fever, ear pain, or respiratory symptoms. In the Pittsburgh study the criteria for a diagnosis of ear infection were: (1) onset within 48 hours preceding the office visit; (2) a symptom assessment score of at least 3 on a scale of 0-14; the symptoms evaluated on a 3 point scale (none, a little, a lot) were: tugging on ear, crying, irritability, difficulty sleeping, diminished activity, diminished appetite, and fever; and (3) the presence of middle-ear effusion, and moderate or marked bulging of the tympanic membrane or slight bulging accompanied by either otalgia or marked erythema of the membrane. This is, in fact, admirably rigorous.
The problem, however, is that out in the real world of general practice, primary care physicians do not do all this. Their history is very brief, no symptom scores are assessed, the ears are looked at very quickly, and lots of cases are diagnosed as ear infections that have no actual bulging of the tympanic membrane. What this means is that the group of patients being treated in ordinary offices is significantly different, probably with milder disease, than the patients included in the study. Thus we do not know if the conclusion from the formal study should apply to children with less severe illness.
Clinical "failure" was strictly defined as either a lack of clinical improvement (and this is what parents really care about) or worsening of signs on otoscopic examination (which parents don't care about). My perspective as a practicing physician is that, if the child is not having any symptoms, I don't care what the ear drum looks like. I would never extend or repeat an antibiotic just because the ear drum looked abnormal, whether more so or not. What matters is how the patient is doing.
Finally, both studies arbitrarily chose to use an advanced antibiotic (Augmentin). This is a powerful (probably more powerful than one needs) and effective antibiotic, but it causes a very high rate of gastrointestinal side-effects. In one studied it caused diarrhea in almost half of the children treated. This would mean that treatment is like trading one problem (an ear infection) for another (diarrhea), and it is hard to say which is worse. I can tell you which is messier. Certainly there is a need for additional studies, if we are going to making a recommendation to change general practice, to determine which antibiotic will cause the least side-effects while retaining most of the effectiveness. There are many good candidates.
Thus in my opinion these studies don't change anything. It still comes down to a close call whether young children with mild ear infections should be treated. This decision should be made by the parents, not by the doctor. The doctor's role is to continue to give parents the benefits of the latest information and help them to make a reasonable decision.
Another strategy that has been well-defined as safe and effective in multiple studies is for the physician not to treat at the time of the first visit, but to give a prescription for an antibiotic to use if the symptoms become worse or do not resolve in 2-3 days. This was called a "delayed prescription" for an antibiotic. Only about 50% of parents given a "delayed prescription" actually get them filled, which means that many, many children get better all by themselves. This strategy significantly reduces the use of antibiotics and thus will lead to less emergence of antibiotic resistance among common bacteria. I use this strategy a lot.
IS IT LOGICAL TO PROPHYLAX AGAINST DVT IN HOSPITALIZED PATIENTS? Evidence-based Practice did a nice review of the topic in its June 2010 issue.(6) The basic question is--Do we prophylax everyone, no one, or a selected subset basic on objective criteria? I was very early to jump on this bandwagon (around 1989) but now find myself growing increasingly skeptical. Here are the relevant data. A 2007 meta-analysis of RCTs analyzed a total of 12,391 medically ill patients (mostly CHF, respiratory disease, and/or infection) who received DVT prophylaxis with LMWH, unfractionated heparin, or placebo. Both active drugs reduced the risk of DVD events by 40% compared with placebo with an NNT of 74, and reduced all venous thromboembolism by 41% with an NNT of 87. Pulmonary embolism events, however, were unchanged. Another 2007 meta-analysis of RCTs with 19,958 hospitalized medical patients found that anticoagulant prophylaxis was associated with a significant reduction in PE (RR=0.43) with an NNT of 345, and fatal PE by 62%) with an NNT of 400.
A retrospective analysis of an RCT in 2007 showed that prophylaxis led to a significant reduction in the primary endpoint of DVT, PE, or sudden death in patients with infectious disease (RR=0.46) and age > 75 years (RR 0.52). The relative risks for heart failure and respiratory failure failed to achieve statistical significance.
A 2008 evidence-based guideline from the ACCP recommended prophylaxis with LMWH, unfractionated ed heparin, or fondaparinux for "acutely ill medical patients admitted to the hospital with congestive heart failure or severe respiratory disease, or who are confined to bed and have 1 or more additional risk factors, including active cancer, previous VTE, sepsis, acute neurological disease, or inflammatory bowel disease."
ESTABLISHED RISK FACTORS FOR VTE
Acute infection
Congestive Heart Failure
Previous DVT
Acute respiratory disease Age > 75 yeas
Inflammatory Bowel Disease
Immobility
Lower extremity paresis Obesity (BMI > 30)
Central venous catheterization
Cancer
Nephrotic syndrome
Estrogen therapy (OC, HRT)
Thombophilia, inherited or acquired
Pregnancy, postpartum period
Recent surgery
Recent trauma
COMMENT: What I am seeing in practice is a trend toward giving every patient who is admitted DVT prophylaxis regardless of age or risk factors. That's the way Kaiser does it. The relative risk reductions have tended to be large, although inconsistently reported, but the absolute risk reductions are small (the NNTs are quite high). If you're avoiding pulmonary embolism or death, that's a major benefit and we can tolerate a higher NNT, but these outcomes are inconsistently reported as well. We have this nice list of risk factors, which seem reasonable, but no one appears to be using them. The real work for the future is to quantitate how many risk factors, or what severity of an individual risk factor, turns DVT prophylaxis into a bargain.
REFERENCES:
1. Radkay L, Rodriguez JE. Evidence-based practice 13 No 6: 10-11, 2010; reviewing Lutters M, Vogt-Ferrier NB. Antibiotic duration for treating uncomplicated, symptomatic lower urinary tract infections in elderly women. Cochrane Database Syst Rev. 2008;(3):CD001535.
2. Kelley J, Evidence-based Practice 2010; 13 No 6: 8; reviewing Kyriakidou KG et al. Short- versus long-course antibiotic therapy for acute pyelonephritis in adolescents and adults: a meta-analysis of randomized controlled trials. Clin Ther 2008; 30(10): 1859-68. ACOG Practice Bulletin No 91: Treatment of urinary tract infections in nonpregnant women. Obst Gynecol 2008; 113(3): 785-94.
3. Hoberman A et al. (Pittsburgh) Treatment of acute otitis media in children under 2 years of age. NEJM 2011; 364:105-15.
4. Tahtinen PA et al. A placebo-controlled trial of antimicrobial treatment for acute otitis media. NEJM 2011; 364: 116-26.
5. Klein JO. Is acute otitis media a treatable disease? (editorial) NEJM 364: 168-9.
6. Lyon C. Evidence-based Practice 2010; 13 No 6: 7; reviewing Geerts WH et al. ACCP. Chest 2008; 133(6 suppl):381S-453S. Kanaan AO et al. Meta-analysis of venous thromboembolism in medically ill patients. Clin Ther 2007; 29(11): 2395-2405. Dentali F et al. Ann Intern Med 2007; 146(4):278-88. Cohen AT et al., for the PREVENT Medical Thromboprophylaxis Study Group. Vasc Med 2007; 12(2): 123-7.
COMMENT: To all this I have to say, "Not so fast!" First, the authors used, as is appropriate for a formal study, a "strict" definition of an ear infection. In the Finnish study, three overall criteria were required for the diagnosis of acute otitis media (see videos 1, 2, and 3). First, middle-ear fluid had to be detected by means of pneumatic otoscopic examination that showed at least two of the following tympanic-membrane findings: bulging position, decreased or absent mobility, abnormal color or opacity not due to scarring, or air–fluid interfaces. Second, at least one of the following acute inflammatory signs in the tympanic membrane had to be present: distinct erythematous patches or streaks or increased vascularity over full, bulging, or yellow tympanic membrane. Third, the child had to have acute symptoms, such as fever, ear pain, or respiratory symptoms. In the Pittsburgh study the criteria for a diagnosis of ear infection were: (1) onset within 48 hours preceding the office visit; (2) a symptom assessment score of at least 3 on a scale of 0-14; the symptoms evaluated on a 3 point scale (none, a little, a lot) were: tugging on ear, crying, irritability, difficulty sleeping, diminished activity, diminished appetite, and fever; and (3) the presence of middle-ear effusion, and moderate or marked bulging of the tympanic membrane or slight bulging accompanied by either otalgia or marked erythema of the membrane. This is, in fact, admirably rigorous.
The problem, however, is that out in the real world of general practice, primary care physicians do not do all this. Their history is very brief, no symptom scores are assessed, the ears are looked at very quickly, and lots of cases are diagnosed as ear infections that have no actual bulging of the tympanic membrane. What this means is that the group of patients being treated in ordinary offices is significantly different, probably with milder disease, than the patients included in the study. Thus we do not know if the conclusion from the formal study should apply to children with less severe illness.
Clinical "failure" was strictly defined as either a lack of clinical improvement (and this is what parents really care about) or worsening of signs on otoscopic examination (which parents don't care about). My perspective as a practicing physician is that, if the child is not having any symptoms, I don't care what the ear drum looks like. I would never extend or repeat an antibiotic just because the ear drum looked abnormal, whether more so or not. What matters is how the patient is doing.
Finally, both studies arbitrarily chose to use an advanced antibiotic (Augmentin). This is a powerful (probably more powerful than one needs) and effective antibiotic, but it causes a very high rate of gastrointestinal side-effects. In one studied it caused diarrhea in almost half of the children treated. This would mean that treatment is like trading one problem (an ear infection) for another (diarrhea), and it is hard to say which is worse. I can tell you which is messier. Certainly there is a need for additional studies, if we are going to making a recommendation to change general practice, to determine which antibiotic will cause the least side-effects while retaining most of the effectiveness. There are many good candidates.
Thus in my opinion these studies don't change anything. It still comes down to a close call whether young children with mild ear infections should be treated. This decision should be made by the parents, not by the doctor. The doctor's role is to continue to give parents the benefits of the latest information and help them to make a reasonable decision.
Another strategy that has been well-defined as safe and effective in multiple studies is for the physician not to treat at the time of the first visit, but to give a prescription for an antibiotic to use if the symptoms become worse or do not resolve in 2-3 days. This was called a "delayed prescription" for an antibiotic. Only about 50% of parents given a "delayed prescription" actually get them filled, which means that many, many children get better all by themselves. This strategy significantly reduces the use of antibiotics and thus will lead to less emergence of antibiotic resistance among common bacteria. I use this strategy a lot.
IS IT LOGICAL TO PROPHYLAX AGAINST DVT IN HOSPITALIZED PATIENTS? Evidence-based Practice did a nice review of the topic in its June 2010 issue.(6) The basic question is--Do we prophylax everyone, no one, or a selected subset basic on objective criteria? I was very early to jump on this bandwagon (around 1989) but now find myself growing increasingly skeptical. Here are the relevant data. A 2007 meta-analysis of RCTs analyzed a total of 12,391 medically ill patients (mostly CHF, respiratory disease, and/or infection) who received DVT prophylaxis with LMWH, unfractionated heparin, or placebo. Both active drugs reduced the risk of DVD events by 40% compared with placebo with an NNT of 74, and reduced all venous thromboembolism by 41% with an NNT of 87. Pulmonary embolism events, however, were unchanged. Another 2007 meta-analysis of RCTs with 19,958 hospitalized medical patients found that anticoagulant prophylaxis was associated with a significant reduction in PE (RR=0.43) with an NNT of 345, and fatal PE by 62%) with an NNT of 400.
A retrospective analysis of an RCT in 2007 showed that prophylaxis led to a significant reduction in the primary endpoint of DVT, PE, or sudden death in patients with infectious disease (RR=0.46) and age > 75 years (RR 0.52). The relative risks for heart failure and respiratory failure failed to achieve statistical significance.
A 2008 evidence-based guideline from the ACCP recommended prophylaxis with LMWH, unfractionated ed heparin, or fondaparinux for "acutely ill medical patients admitted to the hospital with congestive heart failure or severe respiratory disease, or who are confined to bed and have 1 or more additional risk factors, including active cancer, previous VTE, sepsis, acute neurological disease, or inflammatory bowel disease."
ESTABLISHED RISK FACTORS FOR VTE
Acute infection
Congestive Heart Failure
Previous DVT
Acute respiratory disease Age > 75 yeas
Inflammatory Bowel Disease
Immobility
Lower extremity paresis Obesity (BMI > 30)
Central venous catheterization
Cancer
Nephrotic syndrome
Estrogen therapy (OC, HRT)
Thombophilia, inherited or acquired
Pregnancy, postpartum period
Recent surgery
Recent trauma
COMMENT: What I am seeing in practice is a trend toward giving every patient who is admitted DVT prophylaxis regardless of age or risk factors. That's the way Kaiser does it. The relative risk reductions have tended to be large, although inconsistently reported, but the absolute risk reductions are small (the NNTs are quite high). If you're avoiding pulmonary embolism or death, that's a major benefit and we can tolerate a higher NNT, but these outcomes are inconsistently reported as well. We have this nice list of risk factors, which seem reasonable, but no one appears to be using them. The real work for the future is to quantitate how many risk factors, or what severity of an individual risk factor, turns DVT prophylaxis into a bargain.
REFERENCES:
1. Radkay L, Rodriguez JE. Evidence-based practice 13 No 6: 10-11, 2010; reviewing Lutters M, Vogt-Ferrier NB. Antibiotic duration for treating uncomplicated, symptomatic lower urinary tract infections in elderly women. Cochrane Database Syst Rev. 2008;(3):CD001535.
2. Kelley J, Evidence-based Practice 2010; 13 No 6: 8; reviewing Kyriakidou KG et al. Short- versus long-course antibiotic therapy for acute pyelonephritis in adolescents and adults: a meta-analysis of randomized controlled trials. Clin Ther 2008; 30(10): 1859-68. ACOG Practice Bulletin No 91: Treatment of urinary tract infections in nonpregnant women. Obst Gynecol 2008; 113(3): 785-94.
3. Hoberman A et al. (Pittsburgh) Treatment of acute otitis media in children under 2 years of age. NEJM 2011; 364:105-15.
4. Tahtinen PA et al. A placebo-controlled trial of antimicrobial treatment for acute otitis media. NEJM 2011; 364: 116-26.
5. Klein JO. Is acute otitis media a treatable disease? (editorial) NEJM 364: 168-9.
6. Lyon C. Evidence-based Practice 2010; 13 No 6: 7; reviewing Geerts WH et al. ACCP. Chest 2008; 133(6 suppl):381S-453S. Kanaan AO et al. Meta-analysis of venous thromboembolism in medically ill patients. Clin Ther 2007; 29(11): 2395-2405. Dentali F et al. Ann Intern Med 2007; 146(4):278-88. Cohen AT et al., for the PREVENT Medical Thromboprophylaxis Study Group. Vasc Med 2007; 12(2): 123-7.